|
Screening for Breast Disease |
|
|
Guide to
Clinical Preventive Services |
 If there were no such thing as breast cancer, there would be little need
to screen individuals for breast disease. Breast cancer is the issue
that drives all breast screening programs.
If there were no such thing as breast cancer, there would be little need
to screen individuals for breast disease. Breast cancer is the issue
that drives all breast screening programs.
The primary strategy involves a three-armed effort: Periodic (annual) professional breast examination, monthly self-breast examination, and mammography at appropriate intervals.
Assumptions
The underlying assumption of all breast screening programs is that
if we can detect a breast malignancy when it is very small, then the
outcome will be better for the patient than if we discover the problem
when it is bigger. Just how true that assumption is and the exact
parameters of that truth are still under debate, as is the effectiveness
of any of the breast cancer screening programs in improving outcome for
women with breast cancer.
Breast Examination
Once a year, a woman's breasts should be evaluated by a qualified health
professional. Any significant abnormalities in texture, contour, skin,
any palpable masses, retractions, dimpling or nipple discharge will
require followup appropriate for the abnormality. Professional breast
exams are felt to be about 80% reliable in detecting significant breast
abnormalities.
Read more about Professional Breast Examinations
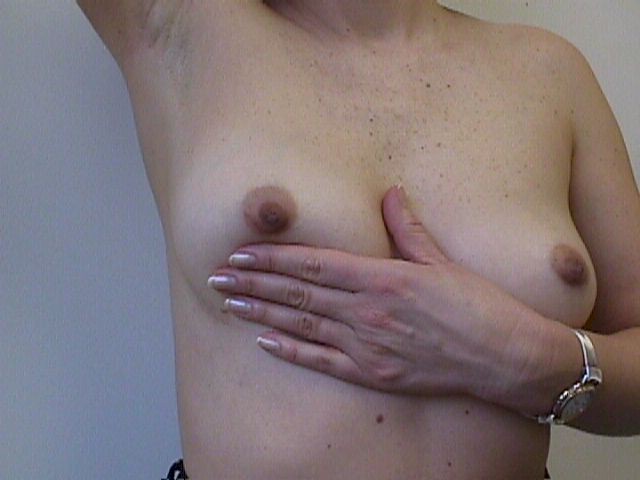
Self Breast Examination
Once a month, a woman should examine her own breasts, looking for
changes in appearance, texture, or nipple discharge that was not
previously present. Examination technique is not obvious, but is a skill
to be learned (and taught). Any new findings should be promptly reported
to the woman's physician or other qualified healthcare provider. Most
breast cancers are first noted by the patient herself.
Some critics of self breast exams have observed that they may cause more problems than they solve. By the time a breast cancer is large enough for the woman to feel herself, it is not likely to be "early." Further, most of the self-discovered breast lumps are benign and do not represent a threat. Nonetheless, they are often subjected to investigation, including biopsy and excision.
Read more about Self Breast Examinations
Mammography
The goal of mammography to to detect very early cancers or pre-cancerous
changes before they have a chance to develop into a more advanced and
dangerous stage. Mammography is felt to be about 80% effective in
detecting significant breast abnormalities, but many of the ones that
are missed by mammography can be detected by examination.
There is controversy over how frequently mammograms should be performed. If there is a clinical abnormality, mammograms can be used to gain additional information about the abnormality (a "diagnostic" mammogram). Many physicians recommend that "screening:" mammograms be performed every other year between ages 40 and 50, and annually thereafter. Some physicians dispute the usefulness of mammograms prior to age 50. Some physicians recommend mammograms more often if there is a strong family history of breast cancer. Some physicians dispute the value of screening mammograms after age 75 or 80. Some physicians dispute the value of screening mammograms at any time.
Breast Ultrasound
Breast ultrasound is used in some countries (although not commonly in
the United States) to screen for breast cancer. It has the advantage
that it is relatively inexpensive, quick, painless, and uses no
radiation. It is particularly good at detecting cystic masses (better
than mammograms). In skilled hands, it does a fair job of detecting
malignancies.
Unfortunately, it is not as good at detecting malignancies as mammograms and so it is not usually used for primary screening in the U.S. It is commonly used in the U.S., however, as an adjunctive method to evaluate abnormalities palpated by the examiner or identified on mammograms.
Thermography
Thermography is a means of looking at the breast with an infrared
(heat-sensitive) imaging device. It relies on the principle that cancers
have increased metabolic activity, generating more heat, that can be
detected with a thermographic process. While this has some theoretical
advantages over other imaging techniques, in practice, thermography has
not been demonstrated to be effective in early detection of significant
lesions, and so is not generally used as a primary screening technique.